A guest blog post by Karen Ashforth, OT MS CLT-LANA.
[This is 14 minute read.]
Thank you for joining us for the third article in the “Understanding Fibrosis” series. In the previous two articles (Part 1 and Part 2), we looked at the basics of fibrosis, its link to lymphedema, and the types of fibrosis and treatment in breast cancer-related lymphedema.
This article will cover phlebolymphedema, the types of fibrosis, and treatments for this population. This information is intended for educational purposes and these treatments should be prescribed and administered by qualified professionals.
What is Phlebolymphedema?
Phlebolymphedema is the most common form of lymphedema in the Western world. It is a combined lymphatic and vascular condition that causes inflammation and lymphedema in the feet and lower legs. It begins with chronic venous insufficiency (CVI) in which the one-way valves in the veins of the lower legs lose the ability to completely close.
While most of the blood normally moves upwards back to the heart, some blood flows backwards because of the faulty valves. This backward flow, called venous reflux, strains the vein walls and blood plasma leaks into the interstitial space. This produces swelling in the feet, ankles, and calves. The lymphatic system works as a safety valve to move the excess fluid out of the legs.
CVI usually affects both legs. At first, CVI symptoms might show up as swollen ankles at the end of the day that reduce overnight when legs are horizontal in bed. As CVI becomes more advanced, it causes lymphatic overload and becomes phlebolymphedema.
In addition to swelling, advanced symptoms of CVI can include wounds, pain, itching, increased susceptibility to infection, varicose veins, and changes in skin color and texture.
What Causes Chronic Venous Insufficiency (CVI)?
There are many contributing factors to CVI. These include family history, pregnancy, inflamed veins, blood clots, trauma, or damage to legs from surgery. Lifestyle factors such as smoking, lack of exercise, prolonged hours of sitting or standing, or being overweight can also impact CVI. Diagnostic testing for CVI includes ultrasound imaging, ankle-brachial index, and various types of venograms. Medical procedures to treat varicose veins may be recommended.
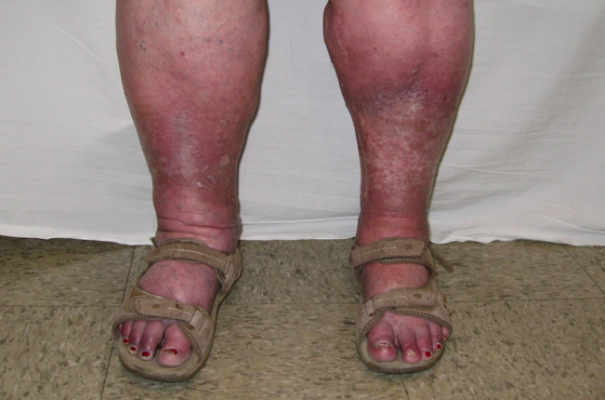
CVI is a Colorful Condition
CVI and phlebolymphedema are common conditions that may be present at the same time as other types of lymphedema. For example, some of my breast cancer-related lymphedema patients also have leg swelling. If CVI symptoms are observed but not treated, an appropriate medical referral should be made. If phlebolymphedema is present, lymphedema treatment should be expanded to address phlebolymphedema.
Any or all of these color changes can be present in phlebolymphedema:
- Brownish-bronze areas are known as hyperpigmentation or hemosiderin staining. This brown discoloration is caused by red blood cells leaking out of the veins and permanently staining the skin.
- Hardened brown patches can appear after a cellulitis infection.
- Star-shaped white scars called atrophie blanche are sometimes left after an infection or healed ulcer.
- Purple varicose veins are visibly enlarged and may be painful. Small red-purple broken venules are called telangiectasia (spider veins.)
- Redness with normal leg temperature that resolves with elevation can be due to vasodilation.
- Redness with heat can be caused by erythema, which is a form of inflammation.
- Red-purple discoloration around the ankles that is accompanied by itching, sores and thickened skin can signal stasis dermatitis.
These ongoing symptoms of redness can often be confused with cellulitis infections, which we’ll address a little later in this article.
Wounds
As CVI progresses, the skin becomes inflamed and fragile and wounds called venous stasis ulcers can form. Because of the environment of poor circulation, these wounds are slow to heal and have a high chance of reoccurring.
Any open wound is vulnerable to developing an infection. It is imperative to make sure wound care is started before beginning treatment for phlebolymphedema and fibrosis.
Risks of Infection
Cellulitis is an infection of the skin, most commonly caused by staph or strep bacteria. One of the functions of the lymph system is to gather and destroy bacteria, and this becomes impaired in lymphedema.
Signs of cellulitis are: redness spreading over an area, hot skin, pain, and increased swelling. People may also experience malaise, similar to coming down with the flu. It is unusual to see cellulitis in both legs. Cellulitis is a potentially life-threatening condition that requires immediate medical attention and treatment with antibiotics.
What is the Best Treatment for Phlebolymphedema?
It is important for patients to have a comprehensive treatment program to reduce swelling and prevent progression of phlebolymphedema. Patients with phlebolymphedema benefit from treatment by wound care specialists and by certified lymphedema therapists.
Complete decongestive treatment is administered by a certified lymphedema therapist. This treatment consists of manual lymphatic drainage, compressive wraps and garments, skin care, and exercise. Conservative treatment consists of elevation, exercise, and compression.
Manual Lymphatic Drainage:
Manual lymphatic drainage is a specialized type of medical massage that increases vascular and lymphatic circulation, and decongests swelling. Modification may be necessary for patient comfort if there is a painful wound present.
Areas of heavy fibrotic damage require more pressure against the surface of dense tissue in order to effectively move swelling that is trapped inside and underneath. Applying compression following manual lymphatic drainage is important to maintaining the reduction of swelling.
Compression:
Wearing compression on the feet and legs helps swelling in a number of ways. External pressure that compresses against the veins improves their ability to move blood upward. This pressure also helps the lymph system. Wearing compression during exercise increases the effectiveness of the calf muscle pump.
Layered bandages or Velcro compression wraps are used in the initial reduction phase of treatment for very swollen feet and legs. They are also used for those with wounds, or for those who have difficulty putting on tight compression stockings. Wound clinics often use disposable compression systems such as zinc oxide wraps or multi-layered Coban wraps over dressings.
Gradient elastic stockings are the most common form of compression. They are generally used in the maintenance phase of treatment. Ready-made stockings have greater pressure at the ankle that lessens towards the top of the stocking, but less pressure in the foot. Custom stockings, wraps, or even tight lace up shoes provide extra compression required for stubborn foot swelling.
Skin care:
First and foremost, all wounds must be treated. Because patients with phlebolymphedema are particularly vulnerable to wounds, prevention is critical. Dry, cracked, and itchy skin is common with phlebolymphedema. Moisturizing the skin heals these symptoms and builds a better barrier to avoid infections.
Exercise:
Walking utilizes the pumping action of the calf muscles to improve circulation in the veins and lymphatic vessels. Even seated exercise can be helpful. Doing ankle pumps for one minute can increase circulation in the legs for thirty minutes.
Ankle flexibility is crucial for proper calf muscle contraction. With tight ankles the calf muscles can’t fully contract as we see in those who “shuffle” when they walk. These people struggle more with swelling because the calf muscle pump is impaired. Those with paralysis or weakness of the lower legs are particularly vulnerable to swelling, however upper body exercise can help increase overall body circulation.
For those without wounds, aquatic exercise gives the benefit of water compression, making muscle contraction more effective. The deeper the water, the better because of greater compression at greater depth: For example, three feet of water creates 67.26 mmHg of pressure on the feet.
Deep abdominal breathing during exercise is also important to activate the diaphragmatic pump, which increases overall blood and lymph circulation.
Elevation:
Elevating the legs uses gravity to help move blood toward the heart. It also assists in the movement of lymph fluid to the lymph nodes in the back of the knees and the groin. These lymph nodes process and filter the fluid so it can eventually exit the body as urine.
Changing the position of the legs from time to time during the daytime is important. Many patients find it helpful to take an afternoon rest in bed with legs elevated on pillows. Some have difficulty lying flat on a bed because of back pain, sleep apnea, or other breathing issues, and prefer a recliner chair for sleep. However, most recliner chairs do not elevate legs horizontally to the level of the heart, leaving legs in a semi-dependent position. A hospital bed can help elevate both the upper body and the legs.
Education:
Patients need to be empowered with education to reduce the risks for swelling and to prevent cellulitis infections. Lifestyle changes make a significant difference with phlebolymphedema. Quitting smoking, losing weight, dietary changes, and regular exercise are all important.
Pneumatic compression:
If phlebolymphedema doesn’t respond adequately to conservative treatment, pneumatic compression should be considered. Pneumatic compression performs both decongestion and compression, and it increases circulation. Pneumatic compression may be used in the clinic and at home to accelerate wound healing and to decrease pain.
While some pneumatic compression systems include the abdomen and hips, most phlebolymphedema patients only require leg compression. During pneumatic compression, the legs are placed inside sleeves that contain individual air chambers and the chambers inflate sequentially up the legs. Each chamber inflates and holds, in a distal to proximal direction, until all chambers are full, preventing backflow of fluid.
Gradient pressure enhances this action by giving greater compression at the feet, and gradually lessening in the higher chambers. Overlapping chambers mimic the overlap of bandage wrapping and further reduce fluid reflux. Patients, especially those with painful wounds or diabetic neuropathy, benefit from rapid inflation, a short cycle time, and long pause time between compression cycles to increase comfort during this treatment. The amount of pressure should also be adjusted to determine that the treatment is both effective and comfortable.
What is Lymphostatic Fibrosis and Why is it Important in Phlebolymphedema?
As we learned in Part 1 of this series, lymphostatic fibrosis is present even in lymphedema that is undetectable to the eye. Lymphostatic fibrosis is caused by an inflammatory process occurring with prolonged swelling. This process converts swelling from a liquid to a gel-like consistency. Over time, and without proper treatment, it can become a dense, solid mass.
The lower extremities, particularly the toes, feet, and ankles, are vulnerable to dense swelling (and hence fibrosis) because of the effects of gravity. This is especially problematic for those who sit with their feet on the floor for prolonged periods with little movement, or those who aren’t able to elevate their feet and legs on a bed at night. With phlebolymphedema, as with all types of lymphedema, treating the underlying swelling prevents the progression of fibrosis, which in turn, prevents the progression of lymphedema.
Let’s look at the types of fibrosis commonly seen in phlebolymphedema.
Upside-Down Champagne Bottle
Lipodermatosclerosis is fibrosis found in the layers of the skin in the lower legs and is commonly seen in CVI. It forms a constrictive band of hard fibrotic tissue around the ankle. This changes the shape of the lower legs to appear like an upside-down bowling pin, or champagne bottle, with small ankles and large, swollen calves.
How Does Kaposi-Stemmer’s Sign Point to Fibrosis?
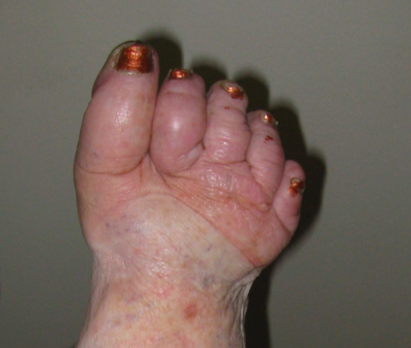 Kaposi-Stemmer’s sign is a clinical test for lymphedema. It is positive when the skin on the top of the second toe (or index finger) is thickened and fibrotic, and the skin cannot lift when it is pinched. This occurs in toes that have developed lymphostatic fibrosis. Over time, chronically swollen toes can enlarge and harden into the shape of shoes, losing the spaces in between like cookies that spread to the edges of the pan. This can also be seen with patients who wear flip flops, sandals, or slippers. The parts of the footwear that are in contact with the body will compress it leaving the uncovered parts to swell.
Kaposi-Stemmer’s sign is a clinical test for lymphedema. It is positive when the skin on the top of the second toe (or index finger) is thickened and fibrotic, and the skin cannot lift when it is pinched. This occurs in toes that have developed lymphostatic fibrosis. Over time, chronically swollen toes can enlarge and harden into the shape of shoes, losing the spaces in between like cookies that spread to the edges of the pan. This can also be seen with patients who wear flip flops, sandals, or slippers. The parts of the footwear that are in contact with the body will compress it leaving the uncovered parts to swell.
Fibrotic Skin Changes in Phlebolymphedema
Chronic swelling can cause changes in the surface and underlying layers of the skin. Hyperkeratosis is when the skin overproduces keratin and becomes thicker. Papillomas are raised wart-like growths, which vary in size from “mossy” patches to large nodules. While lymphedema treatment helps with healing by increasing the circulation in the skin, prescription creams and ointments may also be required.
Post-Cellulitis Fibrosis
Cellulitis infections damage the body by creating fibrotic tissue in the skin, lymphatic vessels, and deep surrounding tissues, which further decreases circulation. It can create a snowball effect of poor circulation, increased swelling and repeated infections. Post-cellulitis fibrosis can become very hard, deep, and dense, and in some cases can feel like a block of wood imbedded in the leg.
How is Fibrosis Treatment Different from Lymphedema Treatment?
Many of the treatments for phlebolymphedema that I’ve described also help fibrosis. However, in cases where fibrosis has become very hardened, specific types of treatment to remodel and soften fibrosis are beneficial. It is important to adjust treatment if there is fragile skin and if there are problems with sensation, such as diabetic neuropathy. Here is a sampling of some types of treatment that help phlebolymphedema fibrosis:
Compression bandaging and garments:
Fibrosis is remodeled by pressure, and the highest comfortable compression gives the best results. Textured, irregular surfaces are especially helpful for softening fibrosis. Examples of this are channeled foam, chipped form pieces that are quilted into pads or garments, and elastic garments with a textured weave. The negative spaces in the surface of the garment are created by the quilting or fabric texture, which directs fluid out of swollen areas. Wearing an elastic sleeve, Velcro wraps, or bandages over chip foam garments or pads provides extra pressure and increases their effectiveness.
As a rule, thicker compression is more effective for both swelling and fibrosis, but it is bulkier, which makes it more awkward to walk. For this reason, bandages over foam are usually only worn day and night during the initial reduction phase of treatment. Some patients continue to use bandages and foam for maintenance use at night, or transition to a chip foam garment. I often recommend knee-high chip foam boots with a zipper or Velcro closure for my phlebolymphedema patients, especially those with paralyzed legs (who sit during the day in wheelchairs) to help stimulate leg circulation and treat swelling and fibrosis.
The harder the surface of the compression, the more aggressive the anti-fibrotic effect. Waffle foam or soft grey foam with channels gives gentler effects than hard foam or chipped foam, which can contain foam pieces of varying density. Pads and garments made from cherry pits are very aggressive and can be highly effective, but should be used cautiously, or avoided in cases of fragile skin or decreased sensation.
Anti-fibrotic elastic compression is easier to wear during the daytime because it is less bulky, but it is less aggressive in treating both swelling and fibrosis. There are many ready-to-wear and custom compression stockings with textured anti-fibrotic weaves. Of particular note are specialized “gloves” worn on the feet that have individual sleeves to compress and even remodel fibrotic toes. They are a great transition from wrapping the toes because they take less time to put on. Be sure to solve wound and fungal issues before using elastic compression on the toes.
Manual therapy:
As mentioned earlier, deeper and more aggressive massage is important to treat fibrotic tissue. Anti-fibrotic massage with specialized tools creates a controlled microtrauma that can quickly remodel fibrotic tissue. Some tools produce a deep massage and others use negative pressure to lift and stretch hardened tissues. A low-level non-thermal laser used in conjunction with these techniques can enhance this process.
Pneumatic compression:
Evidence proves that higher pressures are required to effectively decongest and remodel hardened fibrotic tissue. Current research points to pressure up to 60 mmHg, but having said this, it is important to make sure the amount of pressure is comfortable. Changes in fibrosis and weight gain or loss are reasons to evaluate and adjust pressure. Using quilted compression pads and garments underneath pneumatic compression yields powerful results by giving a “dual massage”.
The Impact of Fibrosis Treatment
Addressing fibrosis has many benefits. It remodels hardened tissues that trap fluid, making it easier to manage swelling. It also makes it easier for people with phlebolymphedema to walk, which increases safety and decreases the risk of falling. The softer tissues have increased circulation, which helps to decrease pain and risk of infections. This treatment helps wound healing and prevents future wounds.
My passion for spreading the word about fibrosis treatment is rooted in my desire to give people hope that it is possible to make positive changes and stop the progression of lymphedema. I dedicate this article to the many patients I have had who started out with rock hard feet and legs that have transformed to butter soft tissues.
In the next article in this series, “Understanding the Impact of Fibrosis in Lipedema,” I’ll discuss the types of fibrosis commonly present in this condition and treatment options.
About the Author
Karen Ashforth, MS, OTR/L, CLT-LANA has practiced as an occupational therapist for 38 years. Specializing as a board-certified hand therapist led to her interest in lymphedema and fibrosis nearly 20 years ago. Karen’s passions in lymphedema practice are equipment innovation and development, treatment of underlying fibrosis and inflammation, and assessment of complex and difficult cases. She is considered an expert in clinical use of pneumatic compression and has participated in development of numerous devices and appliances. She currently works at St. Joseph’s Medical Center in Stockton, California, providing outpatient lymphedema treatment and also has a private consulting practice. Karen speaks frequently at academic, clinical and professional settings and performs clinical research that she presents and publishes nationally and internationally. She is also an adjunct faculty member with the University of the Pacific in the Doctoral Physical Therapy Program.