a guest blog post by Karen Ashforth, OT MS CLT-LANA
This is an 9-minute read.
Thank you for joining us for the second article in the “Understanding Fibrosis” series. In the previous article, "Identifying Fibrosis in Every Stage of Lymphedema," we looked at the basics of fibrosis, its link to lymphedema, and the symptoms that occur during each stage of the progression of lymphedema.
This article will address specific types of fibrosis that affect a breast cancer patient and give examples of treatment.
The Impact of Post-surgical Fibrosis on the Body
Scar tissue is a common and well-known form of fibrosis. Most individuals with breast cancer will have some form of surgery, which has an impact on lymphatic circulation in a number of ways. Surgical scar tissue can form a barricade to normal lymphatic circulation, creating stasis. When lymph nodes are removed it can create further congestion. There are many factors that can influence surgical outcomes: type and extent of surgery, type of surgeon, and whether or not there are other treatments such as chemotherapy or radiation therapy that can compound wound and scar healing.
The Stages of Wound Healing:
Post-operative swelling begins in the inflammatory stage of wound healing 1-2 days after surgery, when neutrophils enter the wound to remove bacteria. Once the wound is cleaned out, tissue grows to close the wound. Swelling and inflammation are a normal part of this process, which reaches its peak at 2-4 weeks after surgery. Post-surgical swelling may take weeks or months to totally resolve, but if lymphedema is developing or already present, swelling can be more profound and persistent. At about 3 weeks after surgery the body moves into the proliferation stage where the wound closes and scar tissue formation begins. Scar tissue is a necessary part of wound healing and will continue to mature for up to 2 years.
What Determines the Severity of Post-surgical Fibrosis?
Scar healing is influenced by the amount of post-surgical swelling and inflammation, which in turn can be worsened by many factors. These include co-morbidities such as diabetes, circulatory or autoimmune conditions. Many medications, including some types of chemotherapy, can create swelling as a side effect. Additionally, some people are genetically predisposed to keloid scar formation, where the body creates a bulky raised scar. Post-surgical complications such as a cellulitis infection or tissue necrosis can also influence and increase scar formation. Development of lymphedema before or after surgery slows wound healing and impacts scarring. Over time, untreated lymphedema can also produce lymphostatic fibrosis. Lymphostatic fibrosis is fatty tissue formed from lymph stasis that impedes circulation, which we learned about in Part 1. Next, let’s look at the effects of radiation therapy which forms a more wide-spread fibrosis, and can complicate scar healing.
What is Radiation-induced Fibrosis?
In addition to treating cancer, radiation therapy alters tissue composition, making tissues thinner, harder and more brittle. Radiation following surgery creates changes to the surgical scar to make it harder and denser, as well as creating fibrotic tissue around the scar. Some of the mechanical factors that influence radiation damage include: type, duration, intensity, amount, and location of the radiation field. There are also patient-oriented factors that affect tissue healing and long term outcomes such as skin sensitivity, tissue density and composition. Radiation therapy can create significant damage in addition to producing fibrosis. Depending upon the area radiated, possible long-term effects include heart disease, osteoporosis and (in cases of head radiation) tooth loss.
Fibrosis and Cording
Cording, also known as Axillary Web Syndrome, can be a painful and debilitating form of fibrosis. Cords are thought to be formed by the hardening of small veins or lymph vessels and occur most commonly between the axilla and the elbow, although they can extend down into the hand or the trunk. Cording can feel and appear like one or more guitar strings just under the surface of the skin.
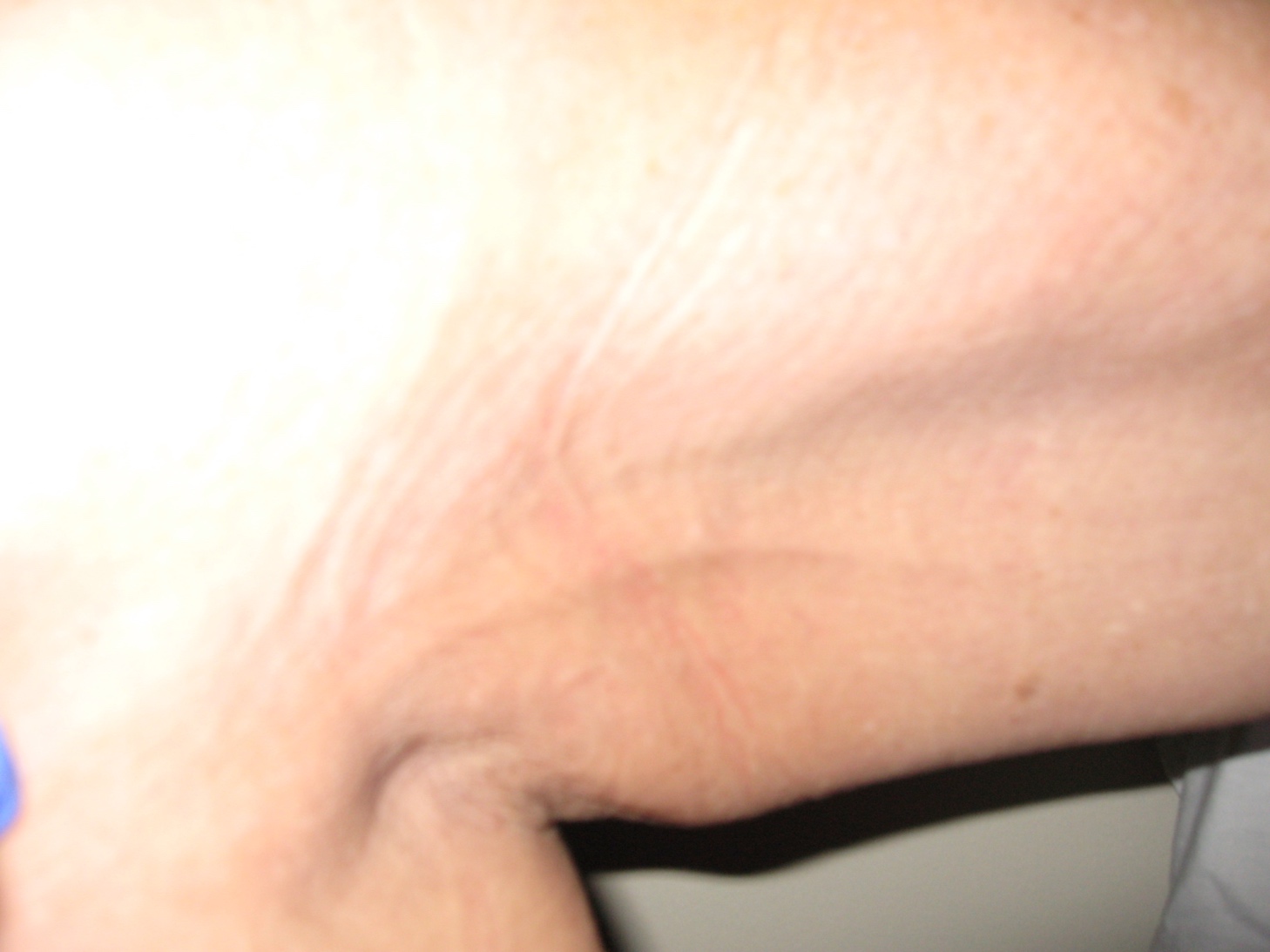 A patient with cording might describe it as a tightness and pain that pulls in the axilla or arm. These patients often lose mobility in that arm which restricts their ability to reach overhead. Sometimes cords will mysteriously resolve on their own. Even though cording isn’t extremely common, it’s common enough that we should be able to identify it and treat it with our patients.
A patient with cording might describe it as a tightness and pain that pulls in the axilla or arm. These patients often lose mobility in that arm which restricts their ability to reach overhead. Sometimes cords will mysteriously resolve on their own. Even though cording isn’t extremely common, it’s common enough that we should be able to identify it and treat it with our patients.
Fibrosis Treatment Options for Breast Cancer Patients
First and foremost, it is important to address any swelling that is present. Congestion can cover and obscure fibrotic tissue, making it more difficult to treat. As we learned in Part I, lymph stasis creates lymphostatic fibrosis which impacts lymphatic circulation and can become a snowballing cycle creating more fibrosis, which can lead to more swelling. Complete decongestive treatment for lymphedema consists of manual lymph drainage, compression, skin care, and exercise. These treatments also form an important foundation for fibrosis treatment by giving patients tools to deal with swelling, and to prevent the progression of lymphedema and fibrosis.
Treatment for lymphedema and fibrosis frequently overlap, but some fibrosis treatments are too intense to use with vulnerable tissues right after surgery and radiation therapy. Gentle treatment is more appropriate while the body takes time to heal sufficiently. If the patient has also had chemotherapy, the body needs an even longer period of healing time to allow the immune system to recover before starting aggressive fibrosis treatment.
Treatment Example:
Breast Cancer Related Lymphedema and Fibrosis
 This example describes many of the types of lymphedema and fibrosis treatments commonly used to help a breast cancer patient. Treatments that are specifically targeted for her fibrosis are in bold italics.
This example describes many of the types of lymphedema and fibrosis treatments commonly used to help a breast cancer patient. Treatments that are specifically targeted for her fibrosis are in bold italics.
A.M. had neoadjuvant chemotherapy and then underwent a R breast lumpectomy with axillary node dissection (2/12 nodes positive for cancer.) During radiation therapy she was referred to lymphedema therapy because the post-surgical swelling of her R arm, axilla, thorax and breast was not going away, and was in fact getting worse.
A.M. received a comprehensive lymphedema evaluation and began Complete Decongestive Treatment. She received manual lymphatic drainage, and her arm was wrapped in bandages. She elevated her arm on a pillow when she slept at night or when she sat on the couch during the daytime. She did simple exercises to improve her shoulder and arm range of motion. She applied cream to the tender skin on her breast and axilla that was provided by her radiation oncologist. She learned about lymphedema risk reduction and how to prevent infections. She transitioned from bandaging to garments that she could easily put on and take off: she wore a compression glove on her hand and a Velcro wrap on her arm (because her arm was too large to comfortably wear an elastic sleeve.) At night she wore a quilted arm sleeve filled with small pieces of chipped foam which she bandaged over to give her arm a gentle micro-massage. After A.M. completed radiation therapy and her skin healed, she began to wear a quilted chip foam pad under a specialized bra to help with her breast swelling and pain, and to create a gentle micro-massage to the scars at her breast and axilla. A.M.’s therapist used a low-level laser while she performed gentle decongestive massage to begin to soften and stretch the scars and radiation fibrosis at her breast, thorax and axilla.
Because the conservative treatment that A.M. was receiving wasn’t enough to significantly reduce her arm swelling, her therapist recommended a pneumatic compression device. Using this specialized lymphedema pump created compression, decongestion and softening of the tissues of her arm, axilla, breast, and thorax. She wore her quilted garments while using the pump for a “dual massage” which furthered the softening of fibrotic tissue and reduction of the swelling in her arm and hand. This helped her to progress from using the Velcro arm wrap to a custom flat knit arm compression sleeve with an antifibrotic weave, which created a mild micro-massage while she wore it.
Two months after she completed her radiation therapy, the burns and wounds on her breast and thorax had completely healed and her hair had grown back from chemotherapy. But the skin and underlying tissue of her breast, thorax, and axilla felt like they were getting harder and “stuck together.” A.M. began to notice several “strings” between her armpit and her elbow that made it difficult for her to lift her arm. Her therapist recommended special pads with cherry pits quilted inside to use in addition to her quilted chip foam garments to accelerate the softening of tissues on her breast and axilla areas. Her therapist also used the low-level laser over these areas while performing anti-fibrotic massage with specialized tools. Some tools produced a deep massage and others which used negative pressure to lift and stretch her hardened tissues. Her therapist suggested that she perform a trial in the clinic to titrate and increase the pressure on her pneumatic device within comfort levels to increase the anti-fibrotic effects. She made sure A.M. was positioning the axilla chamber in her pump appliance correctly, so that when it inflated it decongested and remodeled the fibrotic damage in that hard to reach area.
A.M. started to rapidly feel relief from the tightness and pulling of the surgical, radiation and cording fibrosis in her right upper body. She practiced neural tension exercises that helped the pulling and pain in her arm and she started to feel so much better that she felt ready to join an aquatic decongestion class that was sponsored by her lymphedema clinic. Being in the water helped her swelling and as she built up her stamina and could exercise more, she lost weight, which not only decreased her body mass, but helped to further decrease her lymphedema and fibrosis symptoms.
A.M. continued to use her decongestive and anti-fibrotic tools independently at home and saw her lymphedema therapist for a few visits every six months to upgrade her compression garments, which became loose as she continued to gradually lose weight. She also received “fibrosis tune-up treatments” from her therapist, knowing that her surgical and radiation scar tissue could continue to tighten and mature during the two year window of healing.
Although this case describes a patient during and immediately after cancer treatment, I see many patients who completed treatment 10, 20, and even 30 years ago who are just now being referred for lymphedema. While early treatment always yields the best results because it can prevent the progression of lymphedema and fibrosis, I want to give patients hope. Treatment at any stage can improve symptoms, help the body heal from surgical, radiation-induced, and cording fibrosis, and empower patients with knowledge and tools to self-manage symptoms.
Next Up:
In the next article in this series, “Treatment of Lower Extremity Fibrosis,” we’ll learn about the impact of cellulitis and lipodermatosclerosis on foot and leg lymphedema.
About the Author
Karen Ashforth, MS, OTR/L, CLT-LANA has practiced as an occupational therapist for 38 years. Specializing as a board certified hand therapist led to her interest in lymphedema and fibrosis nearly 20 years ago. Karen’s passions in lymphedema practice are equipment innovation and development, treatment of underlying fibrosis and inflammation, and assessment of complex and difficult cases. She is considered an expert in clinical use of pneumatic compression and has participated in the development of numerous devices and appliances. She currently works at St. Joseph’s Medical Center in Stockton, California, providing outpatient lymphedema treatment and also has a private consulting practice.
Karen speaks frequently at academic, clinical and professional settings and performs clinical research that she presents and publishes nationally and internationally. She is also an adjunct faculty member with the University of the Pacific in the Doctoral Physical Therapy Program.